面向临床手术的激光钻切骨孔微观组织及抗失稳行为
Bone drilling is the most common surgical intervention used to install implants and treat fractures, and the microstructure of bone holes significantly affects fracture stability and the postoperative healing process. Traditional mechanical drilling can easily damage the microstructure of bone holes, produce cracks and bone chips, and seriously affect fracture stability. The contactless interaction of laser beams with bone has attracted increasing interest because it offers greater freedom and higher precision during drilling and provides a promising solution to improve the anti-instability performance of the drilled bone hole for clinical application. However, current studies on bone holes drilled by laser mainly focus on the analysis of macroscopic morphologies of bone cracks; moreover, the microstructure and anti-instability behavior of bone holes drilled by laser concerning heterogeneous structures are rarely investigated. To further promote the clinical application of the laser drilling of bone, this study systematically evaluates the microstructural characteristics and relationship between the microstructure and related anti-instability behavior of bone holes drilled by laser, which is helpful for optimizing the laser drilling strategy and providing guidance for the promotion of the laser drilling of bones for clinical application.
Freshly extracted sheep tibia are selected for in vitro laser bone drilling. A mid-infrared laser with a wavelength of ~2 μm is used to drill 3 mm-diameter bone holes on the sheep tibia. First, the atomic force microscopy (AFM) is used to characterize and compare the elastic modulus distributions of the tissues around the bone holes drilled by a laser with different power densities and by a mechanical drill bit (Fig. 1). The microstructure of the bone-hole tissue is then quantitatively analyzed and evaluated using fractal evaluation. Subsequently, a heterogeneous four-phase composite model is established by considering the heterogeneous bone structure and mechanical properties of the bone hole. The stress distributions of the bone holes drilled by the laser and by mechanical drill bit under the action of axial force are simulated to visualize the anti-instability behavior of the drilled bone holes.
The width of the elastic modulus affected zone around the bone hole decreases with decreasing laser power density (Fig. 2). Under the optimal laser power density of 5.70×104 W/cm2 and scanning speed of 4 mm/s, the width of the elastic modulus affected zone near the bone hole edge is only 200 μm, the width of the elastic modulus affected zone of the hole bone drilled by laser is 67% smaller than that of the bone hole drilled by mechanical drill bit, and the other areas near the bone hole maintain the intrinsic microstructures and mechanical properties of the original bone tissues (Fig. 3). The fractal dimension analysis result shows that the fractal dimension and porosity of the bone tissue near the bone hole drilled by laser are 1.88 and 0.17, respectively, both of which are smaller than those of the mechanically drilled bone hole (Fig. 4). The results indicate that the microstructure of the bone tissue around the laser-drilled bone hole is hardly affected, the intrinsic structure of the bone tissue is maintained, and no cracks are observed on the bone hole wall (Fig. 5). The simulation results show that the stress concentration tendency of the laser-drilled bone hole is lower than that of a mechanically drilled bone hole under the action of axial force, and the cracks are inhibited or deflected around the cement line (Fig. 6), which effectively improve the instability resistance of the bone hole.
In the present study, the microstructural characteristics and anti-instability behavior of laser-drilled bone holes are evaluated using the combination of experiments and simulations. It is found that the elastic modulus of the bone tissue around the bone hole tends to decrease with decreasing power density and increasing distance from the hole wall, and the effect of laser drilling on the elastic modulus distribution around the bone hole is relatively lower than that of mechanical drilling. A quantitative method for evaluating the microstructural morphology under laser action is established based on fractal evaluation, and the fractal dimension and porosity of bone tissue near the laser-drilled bone hole are merely 1.88 and 0.17, respectively, which are almost the same as the intrinsic structure parameters of bone tissue, indicating that laser drilling has a slight effect on the tissue around the bone hole, providing guidance for the optimization of laser drilling parameters. The optimized laser power density and scanning speed is 5.70×104 W/cm2 and 4 mm/s, respectively, for minimal microstructural damage. The width of the elastic modulus affected zone around the bone hole is only 200 μm, which is 67% smaller than that of the mechanical-drilled bone. There are no cracks but open Haversian canals on the bone hole wall. The stress distribution is obtained using the finite element method to visualize the anti-instability behavior of the bone hole. The observed phenomenon reveals that the maximum stress propagates in the interstitial matrix; however, the growth of cracks caused by stress concentration is quite different for the laser- and mechanically-drilled bone holes. The cracks in the laser-drilled bone hole cannot penetrate the cement line, but are inhibited or deflected around the cement line, which improves the instability resistance of the bone hole. Our study shows that laser bone drilling is a new strategy for clinical applications that minimizes microstructural damage and improves fracture stabilization.
1 引言
内固定术是治疗骨折的主要手段,手术中需要进行骨钻孔以提供骨通道,进而安装皮质骨螺钉[1]。皮质骨螺钉的内固定稳定性主要依靠螺钉与骨组织界面间的紧固力。在传统机械钻骨过程中,过大的切削力和扭矩极易损害骨孔的微观组织结构,产生裂纹与骨屑,从而严重影响骨孔的抗失稳破坏能力及愈后效果。Singh等[2]进行了超声振动辅助钻头(RUBD)与普通外科钻头(CSBD)骨钻孔的对比研究,发现RUBD能够减小骨孔壁面的裂纹数量和尺寸,从而提高骨孔的抗失稳破坏能力。然而,RUBD钻骨技术仍属于接触式的机械去除方式,通过转速和进给量的优化无法进一步提升骨孔的抗失稳性能。
激光钻切是一种非接触加工方式,具有更大的自由度和更高的精度,可以通过非接触式去除方式有效降低钻切区域组织的损伤并提高精度[3-5]。近几年随着医工交叉研究的深入推进,激光钻切在骨折治疗等外科手术中的潜在应用优势获得了越来越多的关注[6-9]。Matys等[10]发现,与外科钻头和超声骨刀相比,激光骨钻切可以提高骨孔的精度(孔径和深度),有利于增强微型种植体与骨孔的接合强度。Panduric等[11]在Er∶YAG激光钻切骨孔组织的生物形态学研究中发现,激光钻切可以有效抑止骨孔壁面裂纹的扩展,而且激光钻切骨孔壁面更有利于细胞黏附和浸润,从而促进后期愈合。Robles-Linares等[12-13]测试了机械钻切骨孔周围组织的弹性模量与抗压强度,仿真了皮质骨螺钉从机械钻切骨孔中拔出的全过程,获得了皮质骨螺钉拔出过程中骨孔的应力分布[14-15]。然而,该研究将骨组织简化为各向同性的刚体,并未考虑骨组织的非均质结构特征,不能真实展示骨孔的抗失稳行为。目前,激光钻切骨孔的研究还主要集中在宏观尺度的裂纹扩展行为方面[16],关于骨孔微观组织特征和抗失稳行为的研究鲜有报道。激光钻切骨孔组织微观特征及其抗失稳行为的研究对于正确认识和推进面向临床手术的激光钻切技术具有重要意义。
本文针对激光钻切骨孔,系统分析了不同激光功率密度下骨孔周围组织弹性模量的分布特征,采用分形评价方法量化分析了激光钻切骨孔的微观组织特征,对激光钻切骨孔工艺进行优化,并在充分考虑骨的非均质结构特征的条件下探究了轴向力作用下骨孔的抗失稳行为。研究结果为激光钻切骨孔手术的临床应用提供了参考。
2 试验方法
羊的体重和代谢率与成年人相似[17],因此,本文选取食品工业中的新鲜羊胫骨作为试验材料。试验前对离体生物骨样品进行标准处理[18]。骨组织中的水分对波长为2 μm的中红外激光有更高的吸收率[19],吸收激光能量后水分在极短时间(<1 ms)内蒸发,在骨组织内部引起局部高压,产生“微爆”效应去除骨组织,有效降低热影响,因此本文采用波长为2 μm的中红外激光以旋切法在离体羊胫骨上钻切,获得直径为3 mm的通孔。在本试验条件下,当扫描速度≥4 mm/s,选择激光能量密度为5.70×104、7.33×104、7.74×104、8.15×104、8.84×104、9.17×104 W/cm2时,才能获得无热致碳化的骨通孔,因此选择最优激光参数范围进行对比研究。沿激光钻切骨孔样品中轴切开,分别用于分析骨孔的组织特征和测试骨孔周围组织的弹性模量。
骨孔的微观形貌采用扫描电子显微镜(SEM)进行观察分析。采用原子力显微镜(AFM)在大气和室温条件下测试钻切骨孔周围组织的弹性模量。测试区域自骨孔壁开始,径向总长度为800 μm,如
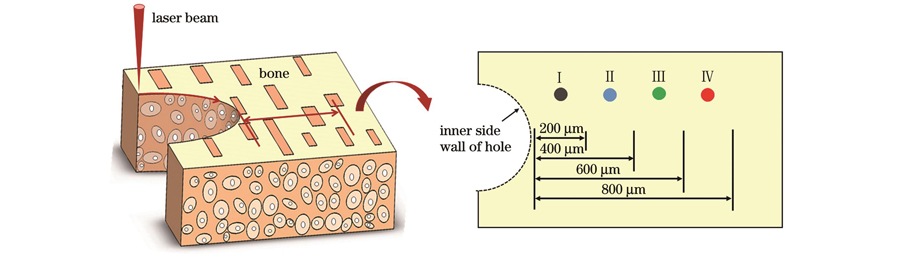
图 1. 激光钻切骨孔周围组织的弹性模量测试位置示意图
Fig. 1. Schematic of elastic modulus test positions of tissues around bone hole drilled by laser
3 分析与讨论
不同功率密度激光钻切骨孔与机械钻切骨孔周围骨组织沿孔径向的弹性模量分布如
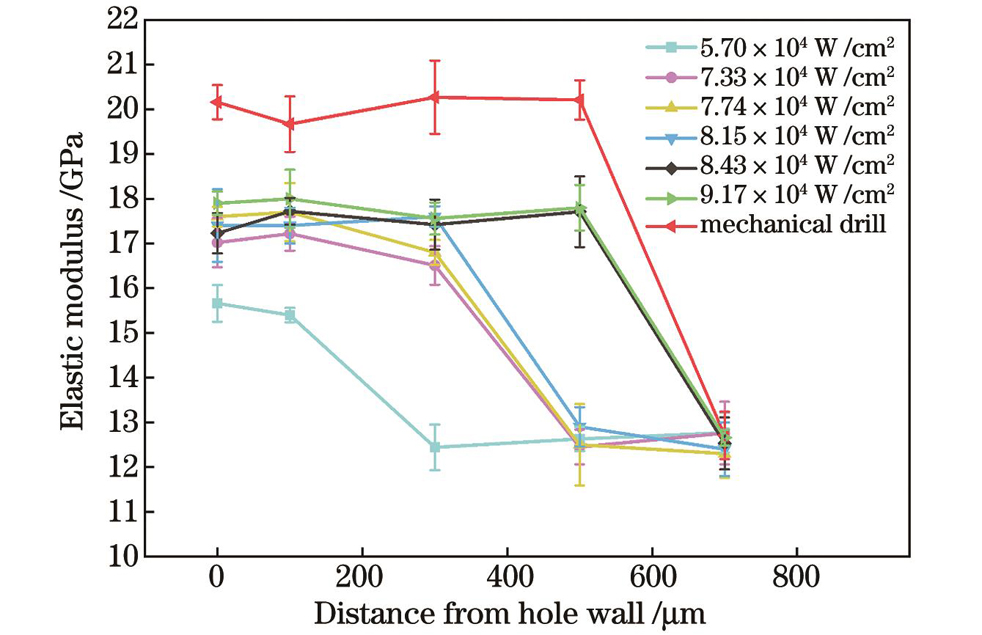
图 2. 不同功率密度激光与机械钻切骨孔周围骨组织的弹性模量分布对比图
Fig. 2. Comparison of elastic modulus distributions of bone tissues around bone holes drilled by lasers with different power densities and by mechanical drill bit
激光钻切骨孔附近I区是骨组织力学特性发生变化的区域,通过对比Ⅰ区与Ⅱ区,进一步分析骨组织微观结构变化对其微观力学特性的影响。
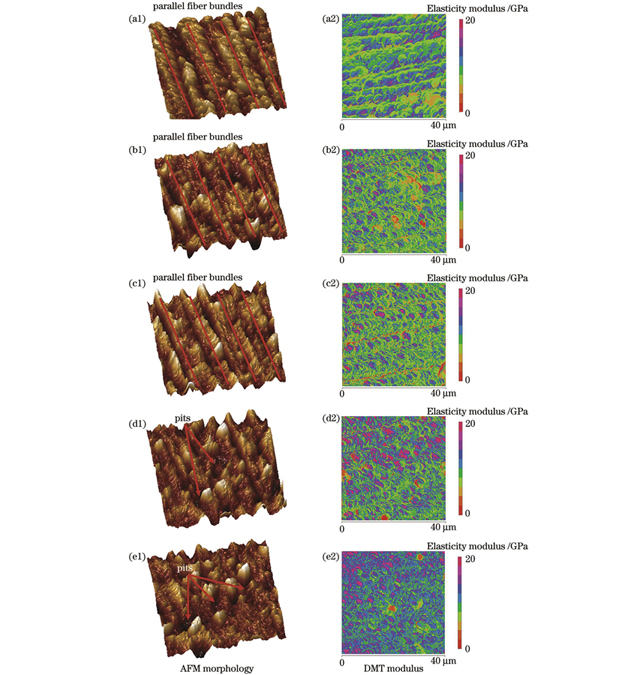
图 3. 激光钻切与机械钻切骨孔周围骨组织的AFM形貌图和DMT模量图。(a1)(a2)原始骨组织;(b1)(b2)激光钻切骨孔附近Ⅰ区;(c1)(c2)激光钻切骨孔附近Ⅱ区;(d1)(d2)机械钻切骨孔附近Ⅰ区;(e1)(e2)机械钻切骨孔附近Ⅱ区
Fig. 3. AFM morphologies and DMT modulus diagrams of bone tissues around bone holes drilled by laser and by mechanical drill bit. (a1)(a2) Intrinsic bone tissue; (b1)(b2) region Ⅰ near bone hole drilled by laser; (c1)(c2) region Ⅱ near bone hole drilled by laser; (d1)(d2) region Ⅰ near bone hole drilled by mechanical drill bit; (e1)(e2) region Ⅱ near bone hole drilled by mechanical drill bit
基于分形理论的自相似原则,可以通过分数维数量化评价材料微观结构的不规则性和复杂性[21],采用分形评价对骨孔周围Ⅰ区与Ⅱ区的骨组织微观结构进行表征,量化分析激光钻切骨孔组织微观结构的变化。AFM形貌图的负深度对应骨组织表面的孔隙,采用盒维数法从骨组织的AFM形貌图中提取相同深度,得到的黑色区域为孔隙面积。分形维数的盒维数[22]为
式中:D为分形维数;δ为以正方形网格边长为元素的递减序列;N(δ)为覆盖目标所需的边长为δ的最小正方形网格数。以黑色区域面积与AFM图像总面积的比值为孔隙率,结果显示,激光钻切骨孔附近Ⅰ区与Ⅱ区骨组织表面的孔隙率均为0.17。根据
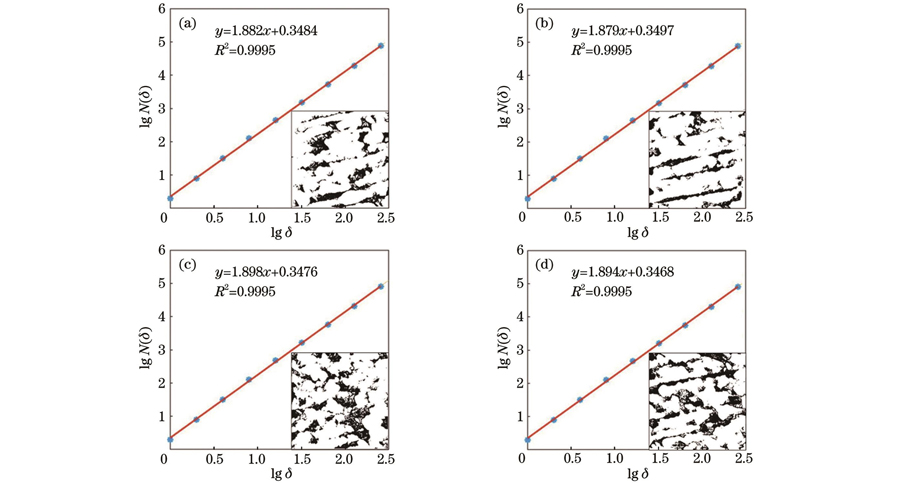
图 4. 基于AFM图像的骨组织分形特征分析。(a)激光钻切骨孔附近Ⅰ区;(b)激光钻切骨孔附近Ⅱ区;(c)机械钻切骨孔附近Ⅰ区;(d)机械钻切骨孔附近Ⅱ区
Fig. 4. Analysis of fractal characteristics of bone tissues based on AFM images. (a) Region Ⅰ near bone hole drilled by laser; (b) region Ⅱ near bone hole drilled by laser; (c) region Ⅰ near bone hole drilled by mechanical drill bit; (d) region Ⅱ near bone hole drilled by mechanical drill bit

图 5. 骨孔壁面的SEM形貌图。(a)激光钻切骨孔;(b)机械钻切骨孔
Fig. 5. SEM images of inner-wall of bone hole. (a) Bone hole drilled by laser; (b) bone hole drilled by mechanical drill bit
根据上述所测得的激光钻切骨孔力学参量,建立轴向拉力作用下皮质骨螺钉紧固于骨组织内部的力学模型,以分析激光钻切骨孔的抗失稳行为。考虑骨微观结构及其材料性能,建立一个由骨单位(osteon)、间质骨基质(interstitial matrix)、骨黏合线(cement line)和Haversian管组成的非均匀四相复合模型[24]。对内置在骨孔内的皮质骨螺钉加载轴向拉力,细化加载区域和骨组织的材料边界上的网格,模型尺寸为2 mm×5 mm,建立的有限元模型如
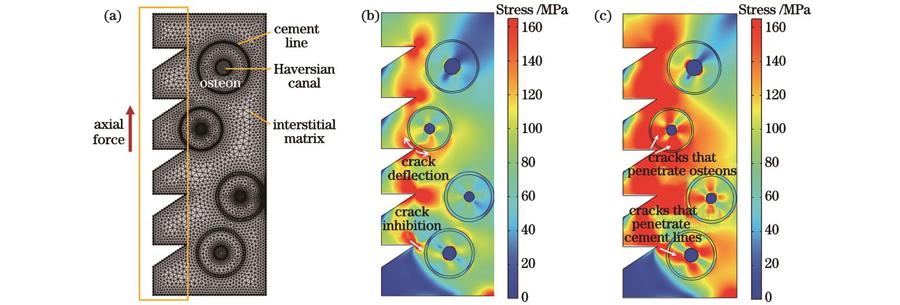
图 6. 轴向力作用下骨孔壁面抗失稳过程的有限元模拟。(a)皮质骨螺钉内置于非均匀四相复合骨组织的有限元模型;(b)激光钻切骨孔应力分布;(c)机械钻切骨孔应力分布
Fig. 6. Finite element simulation of bone hole wall anti-instability under axial force. (a) Finite element model with cortical bone screw inserted in heterogeneous four-phase composite bone tissue; (b) stress distribution in hone hole drilled by laser; (c) stress distribution in bone hole drilled by mechanical drill bit
4 结论
通过试验与模拟相结合的方法,研究了激光钻切骨孔的微观组织特征与抗失稳行为。通过测试分析不同功率密度激光钻切后骨孔的微观结构和周围组织的弹性模量,并结合骨孔微观结构的分形量化评价,发现靠近激光作用区的骨组织分形维数和孔隙率分别为1.88和0.17,骨孔周围骨组织保持了微观结构的本征特征。确定优化的激光功率密度为5.70×104 W/cm2,当扫描速度为4 mm/s时,所获骨孔壁面无裂纹,骨孔边缘弹性模量受影响区域宽度仅为200 μm,比机械钻切骨孔周围弹性模量受影响区域宽度缩小了67%。通过有限元分析对比了激光钻切与机械钻切骨孔在轴向力作用下壁面的应力分布,结果表明,激光钻切骨孔的应力集中倾向显著降低,裂纹沿骨黏合线发生抑止和偏转,骨单位充分起到了屏障作用,增强了激光钻切骨孔的抗失稳能力。研究结果为激光钻切骨的手术临床应用提供了参考。
[1] Tsai Y Y, Chang S W. Pullout strength of triply periodic minimal surface-structured bone implants[J]. International Journal of Mechanical Sciences, 2023, 237: 107795.
[2] Singh R P, Gupta V, Pandey P M, et al. Effect of drilling techniques on microcracks and pull-out strength of cortical screw fixed in human tibia: an in-vitro study[J]. Annals of Biomedical Engineering, 2021, 49(1): 382-393.
[3] 杨强, 季凌飞, 徐博, 等. 皮秒激光微制造As2Se3玻璃红外增透性表面[J]. 光电工程, 2017, 44(12): 1200-1209, 1247.
[4] Han J, Liu Y, Deng Z J, et al. Optimizing noise characteristics of mode-locked Yb-doped fiber laser using gain-induced RIN-transfer dynamics[J]. High Power Laser Science and Engineering, 2021, 9: e36.
[6] 赵海滨, 张先增, 詹振林, 等. 组织表面附着水膜层对脉冲CO2激光骨硬组织消融的影响[J]. 中国激光, 2011, 38(1): 0104002.
[7] 张先增, 郭健, 詹振林, 等. 脉冲CO2激光伴水喷雾的骨组织消融[J]. 光学学报, 2010, 30(7): 2069-2073.
[8] Li C L, Fisher C J, Burke R, et al. Orthopedics-related applications of ultrafast laser and its recent advances[J]. Applied Sciences, 2022, 12(8): 3957.
[9] Song Y, Hu G Q, Zhang Z, et al. Real-time spectral response guided smart femtosecond laser bone drilling[J]. Optics and Lasers in Engineering, 2020, 128: 106017.
[10] Matys J, Flieger R, Tenore G, et al. Er∶YAG laser, piezosurgery, and surgical drill for bone decortication during orthodontic mini-implant insertion: primary stability analysis: an animal study[J]. Lasers in Medical Science, 2018, 33(3): 489-495.
[11] Panduric D G, Juric I B, Music S, et al. Morphological and ultrastructural comparative analysis of bone tissue after Er∶YAG laser and surgical drill osteotomy[J]. Photomedicine and Laser Surgery, 2014, 32(7): 401-408.
[12] Robles-Linares J A, Axinte D, Liao Z R, et al. Machining-induced thermal damage in cortical bone: Necrosis and micro-mechanical integrity[J]. Materials & Design, 2021, 197: 109215.
[13] Zhou Y X, Kastner M J, Tighe T B, et al. Elastic modulus mapping for bovine cortical bone from submillimeter- to submicron-scales using PeakForce Tapping atomic force microscopy[J]. Extreme Mechanics Letters, 2020, 41: 101031.
[14] Chatzistergos P E, Magnissalis E A, Kourkoulis S K. A parametric study of cylindrical pedicle screw design implications on the pullout performance using an experimentally validated finite-element model[J]. Medical Engineering & Physics, 2010, 32(2): 145-154.
[15] 严亚波, 裴国献, 桑宏勋, 等. 螺钉-骨抗拔出力试验有限元模型的建立与验证[J]. 中华创伤骨科杂志, 2013, 15(1): 28-31.
Yan Y B, Pei G X, Sang H X, et al. Screw-bone finite element models for screw pullout simulation[J]. Chinese Journal of Orthopaedic Trauma, 2013, 15(1): 28-31.
[16] Zhang J R, Guan K, Zhang Z, et al. In vitro evaluation of ultrafast laser drilling large-size holes on sheepshank bone[J]. Optics Express, 2020, 28(17): 25528-25544.
[17] McGovern J A, Griffin M, Hutmacher D W. Animal models for bone tissue engineering and modelling disease[J]. Disease Models & Mechanisms, 2018, 11(4): dmm033084.
[18] Ji L F, Zhang L T, Cao L J, et al. Laser rapid drilling of bone tissue in minimizing thermal injury and debris towards orthopedic surgery[J]. Materials & Design, 2022, 220: 110895.
[19] Parker S. Surgical lasers and hard dental tissue[J]. British Dental Journal, 2007, 202(8): 445-454.
[20] Chang Z, Chen P Y, Chuang Y J, et al. Zebrafish as a model to study bone maturation: Nanoscale structural and mechanical characterization of age-related changes in the zebrafish vertebral column[J]. Journal of the Mechanical Behavior of Biomedical Materials, 2018, 84: 54-63.
[21] 陈列, 文关棋, 郭飞, 等. 纳秒激光诱导超疏水硅橡胶表面微结构的分形特性[J]. 中国激光, 2021, 48(6): 0602201.
[22] Kim G J, Yoo H S, Lee K J, et al. Image of the micro-computed tomography and atomic-force microscopy of bone in osteoporosis animal model[J]. Journal of Nanoscience and Nanotechnology, 2018, 18(10): 6726-6731.
[23] O'Brien F J, Taylor D, Clive Lee T. The effect of bone microstructure on the initiation and growth of microcracks[J]. Journal of Orthopaedic Research, 2005, 23(2): 475-480.
[24] Shu L M, Sugita N. Analysis of fracture, force, and temperature in orthogonal elliptical vibration-assisted bone cutting[J]. Journal of the Mechanical Behavior of Biomedical Materials, 2020, 103: 103599.
陈梦雪, 季凌飞, 张犁天, 曹丽杰, 韦杭汝, 孙伟高. 面向临床手术的激光钻切骨孔微观组织及抗失稳行为[J]. 中国激光, 2023, 50(9): 0907207. Mengxue Chen, Lingfei Ji, Litian Zhang, Lijie Cao, Hangru Wei, Weigao Sun. Microstructure and Anti-Instability Behavior of Bone Hole Drilled by Laser for Clinical Surgery[J]. Chinese Journal of Lasers, 2023, 50(9): 0907207.